Related Products
For Professionals
- Amplification
- Assessment of Student Skills, Challenges, Needs
- Early Childhood: Infants, Toddlers, Preschool
- Hearing Loss – Identification, Impact and Next Steps
- IDEA Law Summary Information
- Language and Speech Development Issues
- Legal Issues in Serving Children with Hearing Loss
- Listening (Auditory Skills) Development
- Planning to Meet Student Needs
- Self-Advocacy Skills for Students with Hearing Loss
- Self-Concept: How the Child with Hearing Loss Sees Himself
- Social Skills
- Speech Perception & Learning
Related Teacher Tools Takeout Items
Only One Ear CAN be a Big Deal
About 25-30% of children identified by universal newborn hearing screening have hearing loss in only one ear. This prevalence increases with age to about 1 ½ -2% of the school-age population. Students with unilateral hearing loss are at 10 times the risk for educational challenges as compared to their peers with typical hearing in both ears. Recent research has clarified the issues most likely to be experienced by these children.
Terminology
Unilateral Hearing Loss (UHL) is used to indicate ALL children who have hearing loss in one ear, and specifically for those with useable residual hearing. Single-sided deafness (SSD) is used only for students with severe-profound hearing loss in one ear. These two populations are treated differently for amplification solutions, but ALL of these students require FM/DM devices to improve classroom listening and ‘level the playing field’.
The Heart of the Resulting School Problems for Students with UHL
- Poorer ability to listen and localize sound in noisy environments.

- Even a very low level of noise is likely to interfere with listening, especially when speech is presented toward the poor ear and noise is toward the typically hearing ear.
- The amount of difficulty localizing and processing speech in noise increases with degree of hearing loss.
- These children require speech to be at a higher signal-to-noise ratio if they are to perform similar to normal hearing peers (NH).
- It may take longer for these students to localize the speaker. Some children may benefit from seeing the talker (young children) however the effort required to localize who is speaking may impact the ability to comprehend what was said.
- Children are not always aware that they experience more difficulty listening than peers with NH.
Summary of Research Findings
In October 2017 Phonak held the Unilateral Hearing Loss in Children Conference. The PowerPoints and audio recordings of these presentations have generously been made available by Phonak and the speakers. Go to the following link to view the presentations about UHL in depth: https://www.phonakpro.com/us/en/training-events/events/past-events/2017/uhl-in-children-conference-philadelphia.html
Impact of UHL on Language and School Performance (Judith Lieu)
- The first 2-word phrase occurs at 18 months for UHL versus 15 months for NH.
- Delays in auditory behavior were found in 21% of UHL versus in 4% of NH.
- Delays in preverbal vocalizations were found in 41% of UHL versus only 2.6% of NH.
- Preschoolers ages 4-6 years were found to have delayed language development and have poorer scores on the Children’s Home Inventory of Listening Difficulties (CHILD) checklist.
- Early childhood: the mean total language score = 91.78, almost 10% lower than ‘average’. Converting this difference to age equivalence results in language delays of 6 months for children with UHL. These language findings were not correlated with the severity of the loss or side of UHL.
- Lower scores have been found for syntax, morphology, vocabulary for children with SSD.
- Lower scores on oral language skills, especially oral composite scores (standard score (SS) of 90 vs 99, which was a significant difference).
- Impact of cognitive ability: children with UHL who had a higher IQ (90+) had higher oral skills. Their oral skills improved over time (ages 6-12 years). Children with lower IQ (90 or less) did not improve or improved at a much slower rate in their oral skills over time. Lower IQ UHL students who were on IEPs had oral skills that improved over time whereas those who were not on IEPs decreased in their oral skills relative to age peers over time. (Longitudinal study 2013).
- Academic difficulties are apparent to the teacher: Comparisons of SIFTER checklist scores for students with UHL compared to NH indicated significant differences across SIFTER content areas: Academics – 8 vs 11, Attention – 7.8 vs 12, Communication – 8 vs 11, Class Participation – 9 vs 12.5, School Behavior – 11.5 vs 13.5.
- Quality of life: On the HEAR-QL checklist, children with UHL scored substantially lower than NH (as in scores of 72-80 compared to NH scores of 95).
- Speech/Language Summary: UHL is associated with language delays in young children and school-aged children. There is improvement over time, especially for children with 90+ IQs and those with 90 IQs or less who were on IEPs. Children with UHL do not catch up to the language level of their siblings over time. Risk factors for language delays include: Profound UHL, lower IQ, poverty, maternal education, male.
- Educational Consequences Summary: Children with UHL have an increased risk of grade failure, increased risk to be on IEPs, increased academic weaknesses per teachers, high rates of speech therapy (~50%). Language delays in infancy through adolescence may widen with age and do NOT disappear. Verbal IQ differences may widen with age and do NOT disappear.
Effort and Fatigue Issues for UHL (Ben Hornsby)
- Fatigue can look like tiredness, sleepiness in the morning, inattentiveness and distractibility, mood changes (irritability, frustration), changes in classroom contributions, difficulty following directions.
- Listening-related fatigue may be associated with factors that increase perceived effort. UHL or BHL can increase listening difficulties, which increases listening effort, increases risk for fatigue. This may impact the individual’s evaluation of the effort-reward ratio, meaning when a listening problem is detected the student may initially increase their effort so that they can understand. When, too often, they are not successful in understanding despite the greater effort committed, they can learn that trying harder ‘isn’t worth the effort’.
- As language ability (i.e., as determined by a CELF score) improves, evidence of fatigue secondary to UHL is reduced. Better language = less risk for fatigue.
- Children with UHL who have the largest asymmetry between their ears report the most overall fatigue. SSD likely to have greater fatigue than mild/moderate UHL.
- Adults with UHL were 5 times more likely to report severe fatigue than adults with no hearing loss.
Amplification Findings for UHL
- Younger children (6-9 years) who received their first hearing aid by age 5 showed benefit in localizing sound when they were using the hearing aid in their poor ear (UHL, not SSD). Older children (10-14 years) who received a hearing aid at age 7 or older indicated that the hearing aid was detrimental to localization. Providing early ‘balanced’ hearing to children with usable hearing in the poor ear prior to age 3 provides the best results. Early intervention success was linked to bilateral ‘balanced’ hearing. If a hearing aid is going to be fit, it should happen prior to age 3. Waiting until kindergarten will likely result in rejection (2010).
- Retrospective parent survey results: 72% of parents felt their child improved or greatly improved using a hearing aid in the poorer ear in various listening situations. Of this group of parents, 100% were happy they chose to have their child fit with a hearing aid and 50% expressed that they wished a hearing aid were fit sooner (2002).
Elizabeth Fitzpatrick Phonak presentation:
- At diagnosis, the degree of hearing loss for 154 children with UHL was 31% mild loss, 19% moderate loss, 19% moderate-severe loss, 9% severe loss, 15% profound loss, 7% high frequency loss.
- Based on 337 children, only 21% received amplification shortly after diagnosis. Most take a year or more to get their first hearing device. Average age of diagnosis was 13.9 months; average age at amplification was 42.9 months.
- Of those who received hearing aids, 37% of children with UHL did not use them. (2010)
Erin Picou Phonak presentation:
- This researcher studied whether CROS aids improve speech recognition and comprehension in the classroom. Findings indicated that in comparison to FM use, the benefit of a CROS hearing device is most notable in multi-talker situations with peers who are not using the remote FM microphone. Benefits were most apparent for speech from the ‘bad side.’
Douglas Sladen Phonak presentation:
- Cochlear implants for students with SSD: The most improvement in speech understanding is in the first 3 months after implant activation. Words/sentence scores prior to implantation are about 5% correct. After 3 months they are 35 and 55%, after 6 months they are 40 and 60%, and 12 months post-activation scores are 45 and 65%.
- CI for SSD can improve speech understanding but may have a negligible impact on listening effort.
Intervention for Students with UHL and SSD
- Seating: When possible, the classroom should be arranged in a U-shape, with
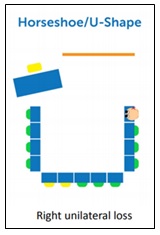 the child’s poor hearing ear facing away from the students.
the child’s poor hearing ear facing away from the students. - Amplification options:
- Roger FM – microphone should be passed during small group activities and discussions (i.e. Touchscreen has automatic omnidirectional mics when in group)
- FM/DM (i.e. Roger Focus) receiver is placed in the typical ear
- Soundfield (CADS) amplification is an option but this does not improve access during noisy group activities. CADS + FM/DM is a good option, but the teacher may have to use 2 microphones.
- Even with optimal amplification, we cannot assume students are fully accessing communication or that they understand and process what they hear.
- Direct teaching:
- Language, syntax, and listening comprehension should be assessed for intervention needs.
- Students need to learn to use their hearing devices and monitor/troubleshoot appropriately.
- Students need to learn self-advocacy skills, including communication repair strategies.
- Students are at risk for identity, self-concept, and social/pragmatic communication skills. They need to connect with other students with UHL to develop a healthy self-concept.
